Leanne Hermes started to experience agonising pain when she got her first period at age 11. In the 33 years since, she's had three babies and 16 surgeries.
Subscribe now for unlimited access.
or signup to continue reading
"I had heavy painful periods; painful sex, bloating, ovulation, urination, bowel movements, back pain. Really every symptom for endometriosis, I had," she said.
"And the pain never went away."
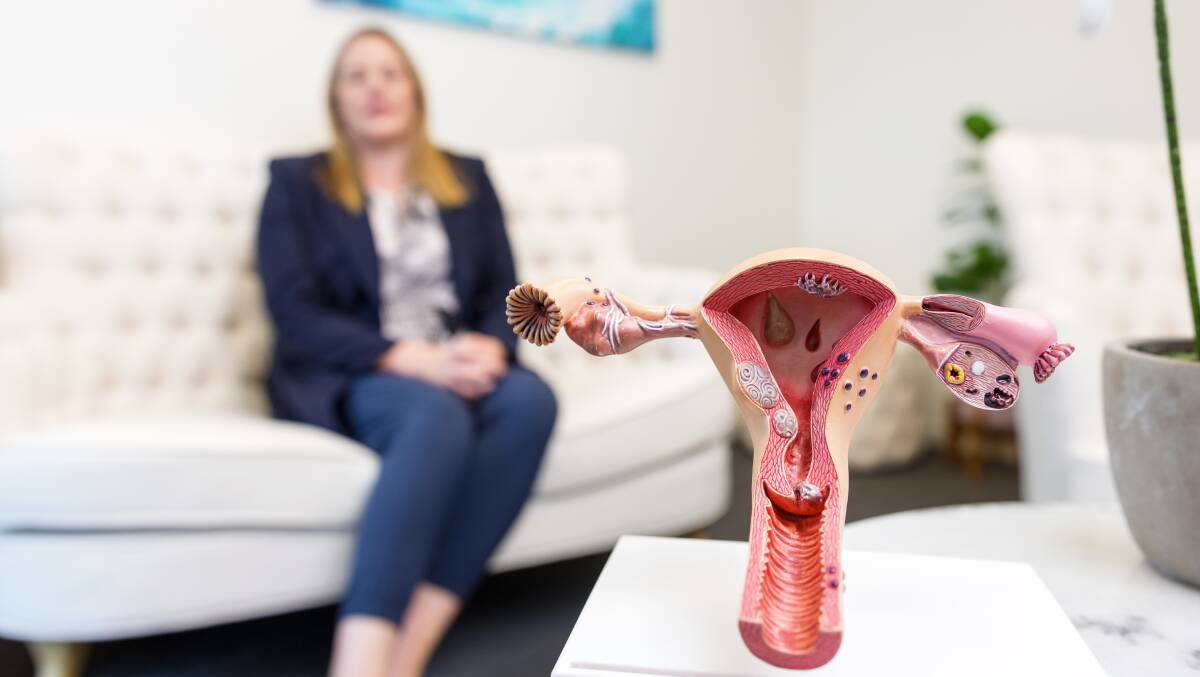
Endometriosis is the presence of endometrium-like tissue outside the uterus. This tissue lines the uterus and is expelled during menstruation. It can be agonising for sufferers, and there is no cure.
After confirming she had the condition through a laparoscopy - an operation that lets a surgeon see the pelvis and abdomen - Ms Hermes said she was put on a pill and told to come back once she wanted to have a baby.
Six months later, the pain was as bad as ever. After each surgery to remove the endometriosis, lesions were found to have grown back.

Progesterone-based contraceptive is the better option for endometriosis, Canberra gynaecologist and laparoscopy surgeon Dr Sarah Broderick said.
"We know that endometriosis is hormonally-driven and estrogen fuels it. Even with extensive [surgery] it can grow back if the ovaries are making estrogen," she said.
While having multiple surgeries to remove endometriosis lesions is not recommended, sufferers can still have significant pain and fatigue after surgery, President of the World Endometriosis Society Professor Luk Rombauts said.
This is because it is not strictly a menstruation or uterus-related disease.
"Lesions are only part of the story" and the condition is understood to affect the immune system, Dr Rombauts said. It causes inflammation and fatigue and can cause immune suppression.

Dr Rombauts said this was why every patient required individualised treatment.
At least one in nine Australians have endometriosis, but experts say it is shockingly under-researched and misunderstood by the public and medical profession.
Things have improved in recent years, the former Coalition government establishing a national action plan in 2018.
The Sexual Health and Family Planning ACT was one of 20 clinics nationwide to receive around $700,000 over four years from the Commonwealth.
The funding will pay for additional healthcare workers and training for ACT doctors, Capital Health Network chief executive Megan Cahill said.
"I think when you talk to women who have the symptoms of endometriosis and pelvic pain, they do find the process of diagnosis really frustrating," she said.
"They'll be dealing with health care professionals that have a high degree of expertise in this area [at the clinic]."
It takes a sufferer seven years on average to be diagnosed, the Australia Institute of Health and Welfare data shows.

For Dickson-based Simone Black it took 20 years, despite having read books about the condition. She had seen GPs and a gynaecologist, but was misdiagnosed with irritable bowel syndrome (IBS).
"I don't have heavy periods, so I [thought], 'I can't have it'," the 31-year-old said.
"It was kind of mind-boggling to me, because I had faith that if I was telling my doctor symptoms that they would be able to diagnose or refer me to someone who would help, but that just never happened."
Dr Broderick said a majority of her endometriosis patients had been diagnosed with IBS.
Symptoms of endometriosis
- Painful periods
- Pain during or after sex
- Abdominal, lower back and pelvic pain
- Pain during ovulation, including pain in your thighs or legs
- Pain when doing a wee or poo
- Pain that gets worse over time
- Pain that stops you from doing things you usually do
- Bladder and bowel problems (e.g. the need to wee frequently, constipation or diarrhoea)
- Bloating around the time of your period
- Tiredness, especially around the time of your period
- Vaginal discomfort
- Mood conditions (e.g. anxiety and depression)
- Source: Jean Hailes Foundation
Her symptoms included leg pain, cyclic sciatica, pelvic floor issues, lower back pain, migraines and severe bloating.
Research has suggested people with endometriosis may be at higher risk of several autoimmune diseases. Ms Black also has psoriatic arthritis, an autoimmune disease, which she said had been taken more seriously by some doctors.
"The pain from [the arthritis] has always been taken far more seriously, but my endometriosis pain is just as bad, if not worse, at times," Ms Black said.

Dr Rombauts admits his profession could better communicate with patients, while Dr Broderick said some medical professionals did not respect women's pain.
"Traditionally ... it was normal for GPs at the front line to tell women, 'It's normal to have pain, it's normal to miss school'," she said.
"[But] you should be able to ovulate without pain. You should be able to have a period without pain."
She said if an initial hormonal treatment, such as the pill, did not work, patients should be referred to a specialist gynaecologist.
A recent campaign by sufferers to change the Royal Australian and New Zealand College of Obstetricians and Gynaecologists (RANZCOG) guidelines for the disease has caused some controversy.
Sufferers are also concerned by the lack of evidence for treatments recommended by RANZCOG. Dr Broderick said this was because of the ethics of control trials, where some people receive treatment but others don't.
"The evidence is really weak because we can't ethically randomise women to have surgery or not ... because it's not ethical," she said.
Endometriosis research was also underfunded, Dr Rombauts said.
"With one in nine people suffering from this condition, how come so much money goes to diabetes research, or prostate research or cardiovascular research [but not for endometriosis]?" he said.
Sufferers like Ms Black believe excisional surgery, where a lesion is completely cut out of the body, is the "gold standard". Ablation surgery is where a lesion is burned.
MORE WOMEN'S HEALTH NEWS:
Dr Rombauts and Dr Broderick both said while they agreed excision-first surgery was appropriate, sometimes ablation was a better alternative.
Evidence also suggests abdominal surgery actually progresses the condition, Dr Rombauts said.
Multiple excision surgeries can create scar tissue which can be more painful than the original endometriosis, he said.
"I've been referred patients for a second opinion after they had multiple repeat surgeries leading to the removal of an ovary because it got entrapped in the scar tissue," he said.

Use of the drug Zoladex, which is also used in cancer treatments, is controversial among some sufferers.
It puts someone in temporary menopause because stopping their period can reduce pain.
It is usually a temporary measure before a patient can have surgery, which may involve a long wait, but is not approved for long-term use, Dr Rombauts said.
The drug should be prescribed for patients with laparoscopy-proven endometriosis, and used only specific cases, Dr Broderick said.
MORE HEALTH NEWS:
The fertility expert said Zoladex does not cause infertility and is used in IVF for women with severe endometriosis.
Endometrioma, the cysts on an ovary, and multiple surgeries to remove ovarian cysts, can reduce egg quality and number, Dr Broderick said.
The former Morrison government committed $2.5 million into reviewing and updating the clinical practice guidelines for endometriosis, a spokesperson for RANZCOG said.


